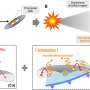
Research is reshaping the understanding of Vitamin D, shifting its classification from a simple nutrient to a crucial hormone with extensive implications for health. Traditionally recognized for its role in preventing rickets and maintaining bone health, Vitamin D is now being acknowledged for its influence on immune function, cancer prevention, and autoimmune diseases. A recent analysis by the MIT Technology Review highlights how this reclassification could lead to significant changes in public health guidelines.
The significance of Vitamin D receptors (VDR) in various tissues suggests that the hormone’s effects extend well beyond the skeleton. Researchers have identified the enzymatic processes necessary for Vitamin D activation in several tissues, including the prostate, breast, and immune cells. This indicates that cells can produce their own active hormones, thereby regulating local growth and immune responses. Foundational research published in Nature Reviews Rheumatology emphasizes that Vitamin D plays a vital role in modulating the innate immune system, serving as a brake on inflammation, which is a key factor in many chronic diseases.
Despite the promising biological mechanisms associated with Vitamin D, large-scale randomized controlled trials (RCTs) have struggled to consistently demonstrate its benefits in the general population. The landmark VITAL trial, which monitored over 25,000 participants, primarily showed null results regarding the prevention of cancer and cardiovascular diseases in a broad cohort. Critics argue the trial’s design was flawed, treating a vitamin like a pharmaceutical. Unlike drugs, Vitamin D exhibits a threshold effect; supplementation may not benefit individuals who already have sufficient levels.
This discrepancy between observational data—indicating strong links between low Vitamin D levels and diseases—and interventional data, which often fails to show significant benefits, complicates public health messaging. The implications are particularly pronounced in cancer mortality rates. While incidence rates appear unaffected by supplementation, mortality data suggests a different narrative. A comprehensive meta-analysis from the German Cancer Research Center indicates that daily Vitamin D3 administration may reduce cancer mortality by approximately 12 percent. The hormone’s ability to inhibit angiogenesis and promote apoptosis in malignant cells contributes to this potential benefit.
The immune-modulating properties of Vitamin D are proving valuable in the study of autoimmune diseases as well. Recent findings published in The BMJ from ancillary studies of the VITAL trial reveal that supplementation can reduce the risk of developing autoimmune diseases by 22 percent, with effects becoming more significant over time. This suggests a cost-effective intervention for conditions such as multiple sclerosis and rheumatoid arthritis, which typically require expensive biologic therapies.
Challenges remain in translating these findings into clinical practice, particularly regarding diagnostic testing. The measurement of 25-hydroxyvitamin D [25(OH)D] is the standard, yet assay standardization is often poor. Common immunoassays can yield inaccurate results due to matrix interference and cross-reactivity. Liquid chromatography-tandem mass spectrometry (LC-MS/MS), while more reliable, is less accessible, complicating the definition of Vitamin D deficiency. The Endocrine Society recommends a threshold of 30 ng/mL, while the National Academy of Medicine suggests 20 ng/mL for bone health, leaving clinicians without a clear target for non-skeletal health issues.
A significant layer of complexity lies in the genetics of Vitamin D metabolism. Research indicates that differing genetic profiles, particularly variations in the CYP2R1 and CYP27B1 genes, affect how individuals respond to Vitamin D supplementation. This variability explains the presence of “non-responders” in clinical trials and points towards a future of precision nutrition. Notably, research featured in JAMA indicates that identifying these genetic variants could enable targeted high-dose therapies for individuals predisposed to rapid Vitamin D catabolism.
Another emerging concept is that of “Free Vitamin D,” which refers to the fraction of Vitamin D that is unbound and biologically active. Research in the Journal of Clinical Endocrinology & Metabolism suggests that assessing free Vitamin D levels may provide a more accurate picture of an individual’s status, potentially resolving cases where patients exhibit low total Vitamin D levels without clinical deficiency symptoms.
The economic implications of these insights could be substantial. If the preventive potential of Vitamin D regarding autoimmune diseases and cancer mortality is validated through further stratified trials, the cost savings for global healthcare systems could be enormous. Current models prioritize expensive treatments for advanced diseases, contrasting sharply with the low-cost nature of Vitamin D supplementation, which costs only a few cents per day.
However, the lack of patentability for natural vitamins presents a challenge for the pharmaceutical industry to fund large-scale, definitive trials needed to shift regulatory consensus. This market failure places the burden of proof on publicly funded research institutions, which often lack the necessary resources for extensive studies. Achieving standardization in assay methodologies and integrating genetic profiling remain critical hurdles as laboratories strive for a universal definition of deficiency that takes bioavailability into account.
Despite these challenges, the industry is pivoting towards developing Vitamin D analogs—synthetic versions designed to separate the calcemic effects from the hormone’s antiproliferative and immunomodulatory properties. By modifying the molecular structure, pharmaceutical companies aim to create targeted therapies for specific tissues, such as prostate or breast tumors, without causing hypercalcemia.
Public interest in Vitamin D is also increasing, driven by the democratization of health information and biohacking communities. The narrative has shifted from simply avoiding rickets to optimizing health and longevity. This consumer demand is leading to a surge in at-home testing kits and innovative delivery systems, though the market is flooded with products of varying quality due to a lack of regulatory oversight.
As the understanding of Vitamin D deepens, it becomes clear that a reductionist view—isolating a single molecule and expecting a straightforward outcome—is inadequate. Recognizing Vitamin D as a pleiotropic hormone necessitates a multidisciplinary approach that encompasses endocrinology, immunology, and genetics. Moving forward, the focus must transition from general population averages to individual biological realities, acknowledging that in the context of steroid hormones, the nuances of each person’s health are paramount. As the mechanisms of action become clearer, the pharmaceutical industry is likely to continue its shift towards developing targeted analogs, paving the way for therapies that respond not just to deficiencies, but to the complex interplay of human biology.