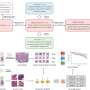
A recent study conducted by researchers at UCL and UCLH has revealed that artificial intelligence (AI) can significantly enhance the ability to predict treatment success in patients with rectal cancer by analyzing standard tissue samples. The research highlights the importance of understanding the immune landscape surrounding tumors, which plays a crucial role in determining patient outcomes and responses to therapy.
The study, published in eBioMedicine, investigated routine pathology images to assess the types and quantities of key immune cells present around rectal cancer tumors. Researchers aimed to determine how these elements of the tumor microenvironment influence survival and the risk of disease recurrence. Traditionally, pathologists manually analyze these images under a microscope, a process that can be labor-intensive and time-consuming.
Dr. Charles-Antoine Collins-Fekete, a senior author of the study from UCL Medical Physics & Biomedical Engineering, emphasized the potential of AI in extracting valuable information from pathology slides swiftly. He stated, “Pathology slides are already part of routine care, so they’re an abundant source of data. We predicted that we could extract valuable information about a patient’s tumor from these slides using AI, which has become very good at analyzing medical images in recent years, and link this to patient outcomes.”
The research team discovered that AI could identify significant immune signals from pathology slides in a matter of minutes. This efficiency stands in stark contrast to slower, more costly techniques such as whole-genome sequencing. The implications of this finding suggest that AI could facilitate more personalized diagnoses and treatments, ultimately leading to improved patient outcomes.
In their analysis, the researchers examined samples from three patient groups, including participants from the ARISTOTLE clinical trial. The findings indicated that patients with higher levels of lymphocytes, a type of immune cell that combats infections and diseases, had better survival rates and a lower likelihood of cancer recurrence. Conversely, patients with increased levels of macrophages—immune cells that can inadvertently promote tumor growth—were associated with poorer outcomes.
Currently, these immune features are not integrated into standard clinical decision-making for rectal cancer. However, the study suggests they could pave the way for more tailored approaches to chemoradiotherapy, enabling identification of patients at greater risk of recurrence.
The AI system utilized in this study was trained on millions of pathology images and tested on 900 patient samples. It effectively measured immune cell levels both before and after treatment. Patients showing an increase in tumor-infiltrating lymphocytes, indicative of a robust anti-tumor immune response, had more favorable outcomes. In contrast, those with tumors that remained immunologically “cold” post-therapy faced a higher risk of earlier recurrence.
Additionally, the research explored how genetic alterations in cancer cells affected immune responses. For instance, patients with an intact KRAS gene and elevated lymphocyte levels exhibited better survival rates than those with KRAS mutations and lower lymphocyte counts. Similarly, high macrophage levels were particularly detrimental for patients with mutations in the TP53 gene.
Dr. Zhuoyan Shen, the first author of the study, noted that while experienced pathologists can recognize some immune features, this information is not routinely utilized in treatment decisions. The AI approach can unveil hidden immune “signatures,” providing insights typically only accessible through expensive and technically challenging methods like whole-genome sequencing.
“By combining immune cell data with genetic information, we can get a clearer picture of how each patient’s cancer will behave before and after treatment,” Dr. Shen explained. This dual analysis could help categorize patients into high and low-risk groups, guiding treatment strategies accordingly.
The researchers also found that tumors exhibiting high mitotic activity, denoting rapid cell division, tended to suppress the immune system, leading to poorer outcomes. This suggests that fast-growing cancers might pose greater challenges for the immune response.
To enhance accessibility for healthcare professionals, the research team has developed a free online tool called Octopath. This platform allows clinicians to upload pathology slides and receive automated immune analyses. While promising, the researchers urge caution, emphasizing the need for further studies to validate their findings in larger and more diverse patient populations, which they plan to pursue in upcoming clinical research.
Professor Maria Hawkins, another senior author from UCL Medical Physics & Biomedical Engineering and a consultant clinical oncologist at UCLH, expressed optimism regarding the potential of AI in cancer classification. She stated, “This is an early step towards the use of AI to aid the further classification of cancer. In the future, clinicians and patients will discuss personalization of treatment using timely information provided by AI. However, further research is required to understand how best to integrate these biomarkers into everyday clinical practice.”
The findings underscore the transformative potential of AI in oncology, particularly in enhancing personalized treatment approaches for rectal cancer patients. As research progresses, the integration of advanced AI tools into clinical settings may significantly improve patient outcomes and treatment efficacy.