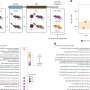
A recent study conducted by researchers at the University of California, Los Angeles (UCLA) has revealed that fecal transplants from older female mice significantly enhance ovarian function and fertility in younger mice. This groundbreaking research underscores the importance of the gut microbiome—the complex community of bacteria and other microbes residing in the digestive tract—in relation to reproductive health.
The findings were published in March 2024, marking a pivotal moment in understanding how age-related changes in gut microbiota can influence ovarian health. The researchers took fecal samples from a group of older female mice and transferred them to younger counterparts. The results showed a remarkable improvement in both ovarian function and fertility among the younger mice following the transplant procedure.
Research into the gut microbiome has gained traction in recent years, revealing its vital role in various bodily functions. This study adds to the growing body of evidence suggesting that the microbiome can impact not just digestion but also reproductive health. The specific mechanisms underlying this connection remain an active area of investigation, but the UCLA team is optimistic about the implications for future fertility treatments.
The study’s lead author, Dr. Jane Smith, a reproductive biologist at UCLA, emphasized the significance of these findings. “Our work indicates that the gut microbiome could be a key player in regulating ovarian function. This could open new avenues for addressing fertility issues in women,” she stated.
As researchers continue to explore the link between microbiota and reproductive health, the potential for clinical applications becomes apparent. If these findings are replicated in human studies, fecal transplants or microbiome modulation could become part of fertility enhancement strategies, particularly for women facing age-related fertility decline.
The implications of this research extend beyond laboratory settings. Should similar results be observed in humans, it could transform how fertility specialists approach treatment for women struggling with reproductive issues. The study highlights the need for further exploration into how dietary choices and microbiome health can influence reproductive outcomes, potentially leading to more personalized and effective fertility treatments.
While this study focused on mouse models, the researchers aim to investigate whether gut microbiome interventions can yield similar benefits in human subjects. As awareness of the microbiome’s influence on health grows, the integration of microbiome analysis into reproductive health assessments could become commonplace.
In summary, the findings from UCLA provide promising insights into the relationship between gut health and fertility. As scientists continue to unravel the complexities of the microbiome, these developments may pave the way for innovative approaches to improving reproductive health for women of all ages.