Researchers have unveiled a biological mechanism that sheds light on why certain lung and ovarian cancers develop resistance to chemotherapy treatments. This finding, published in the journal Nature Aging in September 2023, provides valuable insights into the recurrence of these cancers and their ongoing challenges in treatment.
The study specifically focused on the effects of platinum-based chemotherapies, including cisplatin, on the behavior of tumors in patients with non-small cell lung cancer (NSCLC) and high-grade serous ovarian cancer (HGSOC). Despite the widespread use of these treatments, the long-term effectiveness is often compromised when tumors become resistant or stop responding altogether.
Understanding this resistance is crucial, as NSCLC and HGSOC are among the most common and aggressive forms of cancer worldwide. The research team aimed to identify the underlying biological processes that lead to treatment failure, which has significant implications for improving therapeutic strategies.
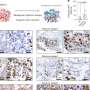
One of the key findings of the study revealed that certain cellular mechanisms enable cancer cells to evade the effects of chemotherapy. The researchers observed that after initial treatment, some cells enter a state referred to as the “zombie cell” effect, where they survive despite the presence of drugs designed to kill them. This state allows the cancer cells to remain dormant for a period before potentially re-emerging as resistant tumors.
The implications of these findings could be transformative for the treatment landscape. By targeting the biological pathways associated with chemotherapy resistance, future therapies may be developed to enhance the effectiveness of existing treatments. This could lead to improved outcomes for patients suffering from these challenging cancers.
In addition to the immediate clinical implications, this research contributes to a broader understanding of cancer biology. It emphasizes the need for ongoing studies to explore how different cancer types respond to various treatments and to identify potential biomarkers for resistance.
As the fight against cancer continues, studies like this one serve as a reminder of the complexities involved in treatment. Understanding the mechanisms of resistance not only aids in developing better therapies but also highlights the importance of personalized medicine in oncology.
Further research will be necessary to translate these findings into clinical practice, but this study lays the groundwork for future advancements in the treatment of NSCLC and HGSOC. The promise of more effective therapies could ultimately change the lives of countless patients facing these devastating diseases.