A groundbreaking study has revealed that a wireless eye implant, known as the PRIMA device, is helping older patients with partial blindness regain some vision. Published in the New England Journal of Medicine, this research focuses on individuals suffering from geographic atrophy, a severe form of dry age-related macular degeneration (AMD). This condition leads to a progressive loss of cells in the macula, the area of the retina responsible for sharp, central vision, ultimately resulting in fuzzy vision and dark patches.
Dr. Frank Holz, the leader of the trial, expressed optimism about the findings, stating, “Late-stage age-related macular degeneration is a dismal disease. Patients are no longer capable of reading, driving a car, watching TV, or even recognizing faces. So [these results] are a game changer in my mind.” The PRIMA device, a tiny chip invented by Daniel Palanker from Stanford University, is currently under development by a neural engineering company based in California.
How the PRIMA Device Works
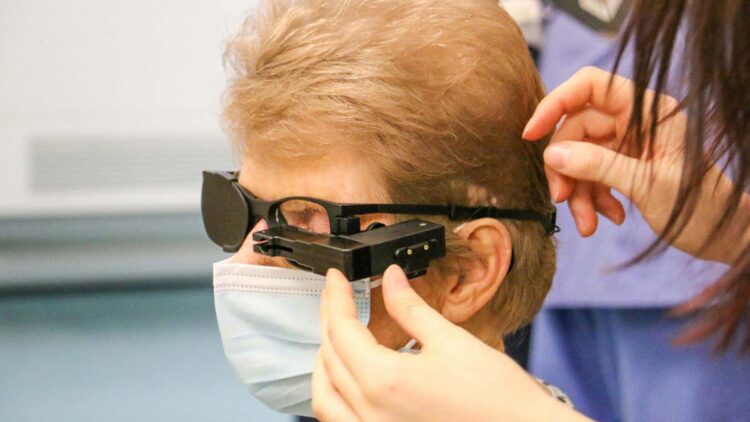
The study involved 38 participants with an average age of 79 years. Each underwent surgery to implant a small wireless chip beneath the retina of one eye. Following this procedure, patients wore augmented reality glasses linked to a portable image processor. These glasses capture images from the wearer’s viewpoint, which are then converted into infrared light and projected onto the chip. The chip transforms this light into electrical signals that stimulate the remaining healthy cells in the macula, allowing the brain to interpret these signals as visual information.
After one year, 32 of the original patients returned for follow-up assessments. Approximately 80% demonstrated significant improvements in vision when the PRIMA system was activated. One of the participants, Sheila Irvine, a 70-year-old, shared her transformative experience: “Before the implant, it felt like I had two black discs in my eyes, with the outside distorted. Now, as a former avid bookworm, I can again read my prescriptions and solve crossword puzzles.”
Challenges and Limitations
Despite these promising results, the implantation process is complex and carries risks. Surgeons must delicately lift the retina’s tissue, and some patients experienced serious side effects, including bleeding and increased intraocular pressure. While most complications resolved within two months, experts caution that not all individuals are suitable candidates for this intricate procedure.
Other eye specialists have responded to the findings with cautious enthusiasm. Dr. Sunir Garg, a retina surgeon, remarked, “Even with new medical therapies, the best that we can do is slow it down. We can’t stop it, and we can’t do anything to bring back lost vision.” He emphasized that while patients may experience some improvements, their overall vision remains poor, limited to black and white, and they require guidance to operate the device.
Dr. Demetrios Vavvas echoed these sentiments, stating, “The limitations are clear. We shouldn’t oversell that the quality of life really improved. But there were certain visual tasks at which the patients were clearly better. It shows us that there is potential in this approach, though it is still, in some ways, a prototype.”
Both Garg and Vavvas expressed the need for further advancements in the technology. Vavvas raised the question of whether patients would feel sufficiently independent with the current capabilities of the device, noting, “We need more than one year of follow-up to see other risks, other problems. Does that signal of efficacy that we see at 12 months remain two years later?”
In response to these challenges, Palanker and his team are already working on an improved chip that will boast a resolution of 10,000 pixels instead of the current 400. This next-generation technology aims to allow patients to perceive gray-scale images, including faces, enhancing their visual experience significantly.
The progress made with the PRIMA device offers hope to those suffering from AMD, marking a significant step forward in the quest to restore vision. While it may not be a complete cure, the potential for improved quality of life for patients is undeniably promising.